- Home
- Fachbereiche
- Neurology
- Stroke care
When stroke strikes,
be ahead of your time.
For stroke patients, time is of the essence. Every minute saved can positively impact patient outcomes.
That’s why it’s key to save time along the entire stroke pathway – from the onset of stroke to treatment and follow-up.
Stroke Quiz
Every minute makes a difference in stroke care.
We are dedicated to supporting healthcare professionals and patients at every stage of the stroke journey. Early recognition and a swift response are essential — because in stroke care, every minute counts. Our advanced diagnostic and therapy solutions empower you to act FAST and enhance patient outcomes. Challenge yourself with our interactive Stroke Quiz and help us spread awareness to save lives.

Webinar recording now available
We are introducing our Solutions for Mobile Stroke Units, designed to speed up decision-making and initiation of treatment: SOMATOM On.site, a CT scanner to aid in diagnosis, and Stroke Connect, a digital all-in-one platform for seamless clinical data exchange, image sharing, and telemedicine.
Follow these patients on their stroke health journeys



Patient stories
Stroke patients tell their stories – about how fast care saved their lives*
Did you know that nearly 60% of all new ischemic strokes happen in people younger than 70, and that 7% occur in people under 44?2
Watch the incredible stories of Stéphane, Zosia, Sebastian, and Gerald – and learn how fast response and treatment can make a difference to a good recovery.
When every second counts, having the right technology matters
Stroke can happen to anyone
Zosia, a 14-year-old student, suffered a stroke during a school day. Her story shows that a rapid response from the surrounding community is critical to the outcome of stroke. Watch her story to learn how Justin Singer, MD, was able to quickly treat and restore blood flow to her brain.
When life gives you a second chance
Stéphane, a father of two, suffered a stroke right after he woke up one morning. Watch the video and find out how the fast reactions of his wife, the paramedics, and the hospital staff played a crucial role in getting the blood flow to his brain restored quickly, leaving him with no disabilities.
From stroke to soccer in just one week
When every second counts, having the right technology matters
Stroke can happen to anyone
Zosia, a 14-year-old student, suffered a stroke during a school day. Her story shows that a rapid response from the surrounding community is critical to the outcome of stroke. Watch her story to learn how Justin Singer, MD, was able to quickly treat and restore blood flow to her brain.
When life gives you a second chance
Stéphane, a father of two, suffered a stroke right after he woke up one morning. Watch the video and find out how the fast reactions of his wife, the paramedics, and the hospital staff played a crucial role in getting the blood flow to his brain restored quickly, leaving him with no disabilities.
From stroke to soccer in just one week
When every second counts, having the right technology matters
Customer stories

Johan Wassélius, MD, PhD, Senior Interventional Neuroradiologist at Skåne University Hospital Lund and Associate Professor at Lund University, Sweden
Improving the stroke pathway in southern Sweden
Distance is a real challenge in Sweden’s southernmost stroke network. Travel time to the nearest hospital can vary drastically. To address this situation Skåne University Hospital and the 13 regional Primary Stroke Centers (PSC) have installed a spoke-and-hub system with a number of procedural adjustments intended to speed up the pathway and improve diagnosis, especially for patients eligible for thrombectomy at the Comprehensive Stroke Center (CSC)*
"At every step of the stroke chain, we try to be as fast as possible [...], to allow the patient to get its treatment as soon as possible of their onset, to achieve the best possible outcome for each patient."
Carlos Molina, MD from Vall d'Hebron hospital in Barcelona
Optimizing the stroke pathway in Barcelona
Carlos Molina, MD, and Alejandro Tomasello, MD, from Vall d'Hebron hospital in Barcelona aim to overcome bottlenecks in the workflow for stroke by using our technology in their one-step approach to stroke treatment. They were able to shorten the door-to-groin time to less than 30 minutes - an important step in improving patient outcomes.

Johan Wassélius, MD, PhD, Senior Interventional Neuroradiologist at Skåne University Hospital Lund and Associate Professor at Lund University, Sweden
Improving the stroke pathway in southern Sweden
Distance is a real challenge in Sweden’s southernmost stroke network. Travel time to the nearest hospital can vary drastically. To address this situation Skåne University Hospital and the 13 regional Primary Stroke Centers (PSC) have installed a spoke-and-hub system with a number of procedural adjustments intended to speed up the pathway and improve diagnosis, especially for patients eligible for thrombectomy at the Comprehensive Stroke Center (CSC)*
"At every step of the stroke chain, we try to be as fast as possible [...], to allow the patient to get its treatment as soon as possible of their onset, to achieve the best possible outcome for each patient."
Carlos Molina, MD from Vall d'Hebron hospital in Barcelona
Optimizing the stroke pathway in Barcelona
Carlos Molina, MD, and Alejandro Tomasello, MD, from Vall d'Hebron hospital in Barcelona aim to overcome bottlenecks in the workflow for stroke by using our technology in their one-step approach to stroke treatment. They were able to shorten the door-to-groin time to less than 30 minutes - an important step in improving patient outcomes.

Johan Wassélius, MD, PhD, Senior Interventional Neuroradiologist at Skåne University Hospital Lund and Associate Professor at Lund University, Sweden
Improving the stroke pathway in southern Sweden
Distance is a real challenge in Sweden’s southernmost stroke network. Travel time to the nearest hospital can vary drastically. To address this situation Skåne University Hospital and the 13 regional Primary Stroke Centers (PSC) have installed a spoke-and-hub system with a number of procedural adjustments intended to speed up the pathway and improve diagnosis, especially for patients eligible for thrombectomy at the Comprehensive Stroke Center (CSC)*
"At every step of the stroke chain, we try to be as fast as possible [...], to allow the patient to get its treatment as soon as possible of their onset, to achieve the best possible outcome for each patient."

Stroke solutions
As your partner in stroke management, we keep you ahead of your time. Our advanced technologies let you speed up stroke care and transform care delivery along the entire pathway – from stroke screening and pre-hospital diagnosis and care to in-hospital diagnosis and treatment and (secondary) stroke prevention to follow-up imaging. Explore our offerings for stroke care!



Care teams need a complete view of patient health data to make timely decisions and reduce time to treatment. eHealth Solutions enable a single view of comprehensive patient health data and make it accessible to care teams and patients across institutions and when needed for fast and confident decision-making. With fast and easy data sharing, eHealth Solutions foster close collaboration across care teams along the entire patient journey to achieve better and timely patient outcomes.
How our eHealth solutions support you
- Care teams can be better equipped thanks to a single view of the longitudinal clinical summary – to better anticipate patient needs along with better patient care
- Immediate access to summarized and most specific patient health data, test results, and diagnostic images in order to adjust care appropriately – reducing time spent searching for information or eliminating unnecessary tests for faster time to treatment
- Elimination of ineffective back-and-forth communication during care transitions through single view of most specific details of patient’s health status
- Aggregation of patient data and easy data sharing among the entire care teams to help better anticipate the patient’s health condition
- Facilitated live video chat communication between physicians to ensure appropriate and collaborative decisions

To confirm ischemic stroke, detect the location of the vessel occlusion, and evaluate the brain damage, you need to rely on excellent diagnostic imaging. CT or MR imaging is considered the gold standard per international stroke guidelines. Our dedicated CT and MRI stroke protocols provide the relevant information on the severity of the damage so you can make confident diagnostic decisions fast.
Our CT and MRI scanners support you with
- Uncompromised image quality throughout the CT scanner portfolio – with optimized signal-to-noise and contrast-to-noise ratios for excellent gray-white matter differentiation and contrast enhancement
- Standardized scanning and post-processing workflow – as well as fully automated or semi-automated perfusion post-processing – to enhance precision medicine
- Fast scan, analysis, and decision support for endovascular mechanical thrombectomy planning, ongoing triage, and treatment pathway: Every second counts in stroke, because time is brain

Our CT scanners provide:
- A highly precise visualization of the penumbra
- Automated 5-step workflow available 24/7
- Neuro Perfusion as routine with zero-click calculation and archiving of perfusion maps

With our MRI scanners, you can:
- Perform a comprehensive stroke work-up including diffusion, perfusion, morphology, and edema identification
- Run fast, push-button and clinically validated brain exams, with GOBrain
- Be one step ahead in acceleration - with Turbo Suite Excelerate including SMS Diffusion

Our ARTIS icono supports in ischemic stroke treatment:
- Twin Spin permits seamless switching between 2D and 3D imaging
- Raising the bar in consistent 3D image quality for whole brain imaging with syngo DynaCT Sine Spin

Our ARTIS pheno supports in hemorrhagic stroke treatment:
- Hybrid OR offers the possibility to perform craniotomy surgery
- syngo DynaCT provides intra-operative confirmation of procedural success
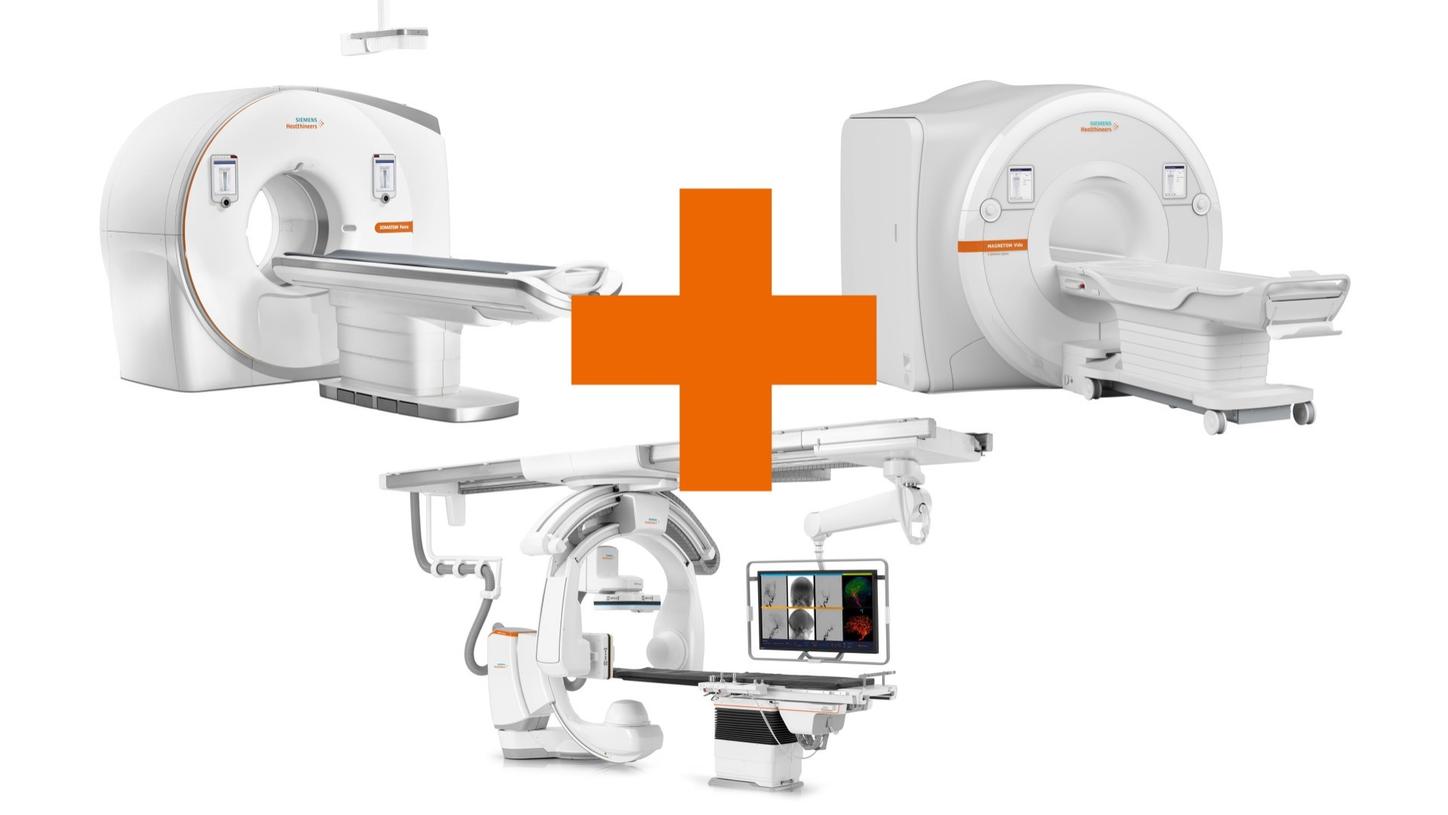
Reducing door-to-groin time for stroke patients at your institution is critical. Optimize clinical processes and perform CT diagnostics and angio stroke treatment in the same room. In our Nexaris Angio-CT suite1), patients can even stay on the same table for diagnostics and treatment – translating into time savings and enhanced safety. In a two-room set-up, you can even use the systems independently.
Nexaris Angio-CT suite: A smart combination of an ARTIS icono biplane and a CT scanner in one room. Speed up diagnostics and interventional stroke treatment by eliminating time spent on transporting and transferring patients.
How our Nexaris Angio-CT suite supports you:- Share one table for diagnostics and treatment, making patient transfer unnecessary
- Potential cost savings thanks to reduced workflow time
- High‐end care for centers of excellence
1)The product shown herein is a customized solution and not commercially available in all countries. Its future availability cannot be guaranteed.
Perform stroke care in the fast lane
Stroke patients need medical help extremely fast. Unfortunately, CT- and MRI-based workflows cost valuable time.1) In an angio-only approach, you may save valuable time by combining pre-procedural imaging and treatment on the same angio system.1)
How our ARTIS icono supports you:
- Our ARTIS icono supports you with fast and precise cone beam CT imaging – right in your angio lab.
- In a stroke emergency setting the door-to-groin time can be shortened by 34 minutes by using syngo DynaCT and the angio only approach.2);3)
- Visualize suspicious intracranial bleedings with syngo DynaCT Sine Spin
- With syngo DynaCT Multiphase it is possible for the first time to visualize cerebral collateral vessels with time-resolved syngo DynaCT, depicting 10 different time points within a period of 60 seconds
“One stop management of stroke patients with suspected large vessel occlusion (NIHSS > 6) is feasible and can save 30 to 60 minutes of in-hospital time.” Marios Psychogios, MDHead of Neuroradiology Department
Marios Psychogios, MDHead of Neuroradiology Department
University Hospital Basel, Switzerland1) Brehm, MN et al.; AJNR. 2019;40(8)1330-1334.
2) M. Psychogios et al.; Stroke. 2017 Nov;48(11):3152-3155.
3) The study was performed at a single center and there can be no guarantee that other customers will achieve the same results.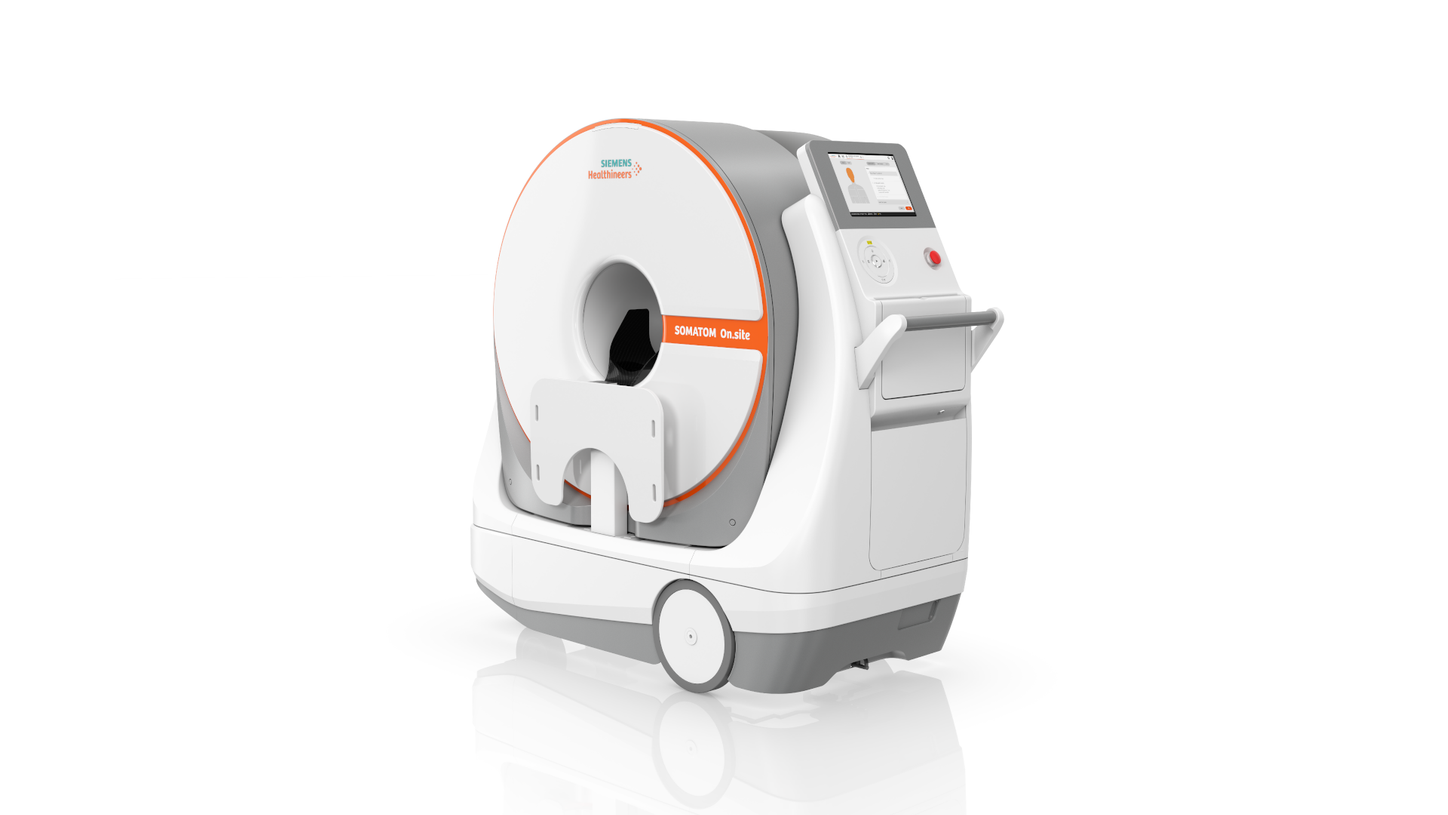
Bring critical care imaging to your patient
One important element in the care of hospitalized stroke patients is follow-up CT imaging. This becomes a time-intensive process if the patient is lying in an intensive care unit (ICU) due to her or his severe condition. Under these circumstances you want your staff to be able to perform diagnostics quickly and make treatment decisions right away and with confidence. Our mobile head CT scanner SOMATOM On.site provides access to consistent and reliable SOMATOM image quality, right at your patient’s bedside.
How our SOMATOM On.site supports you
- Perform in-room scanning with this completely self-shielded CT scanner. This allows staff to stay next to the patient during the examination, and other patients can also remain in the room.
- Reduce patient transports for CT imaging throughout the hospital. This has numerous benefits, from less potential for clinical complications during patient transport to decreased risk of hospital-acquired infections.
- Optimize staff deployment by letting ICU staff stay in their ward and continue to care for ICU patients. With our mobile CT scanner, there is no need for them to accompany patient transports for head CT examinations.
- Achieve high image quality at the point of care and rely on SOMATOM components like Stellar detector and SAFIRE iterative reconstruction.
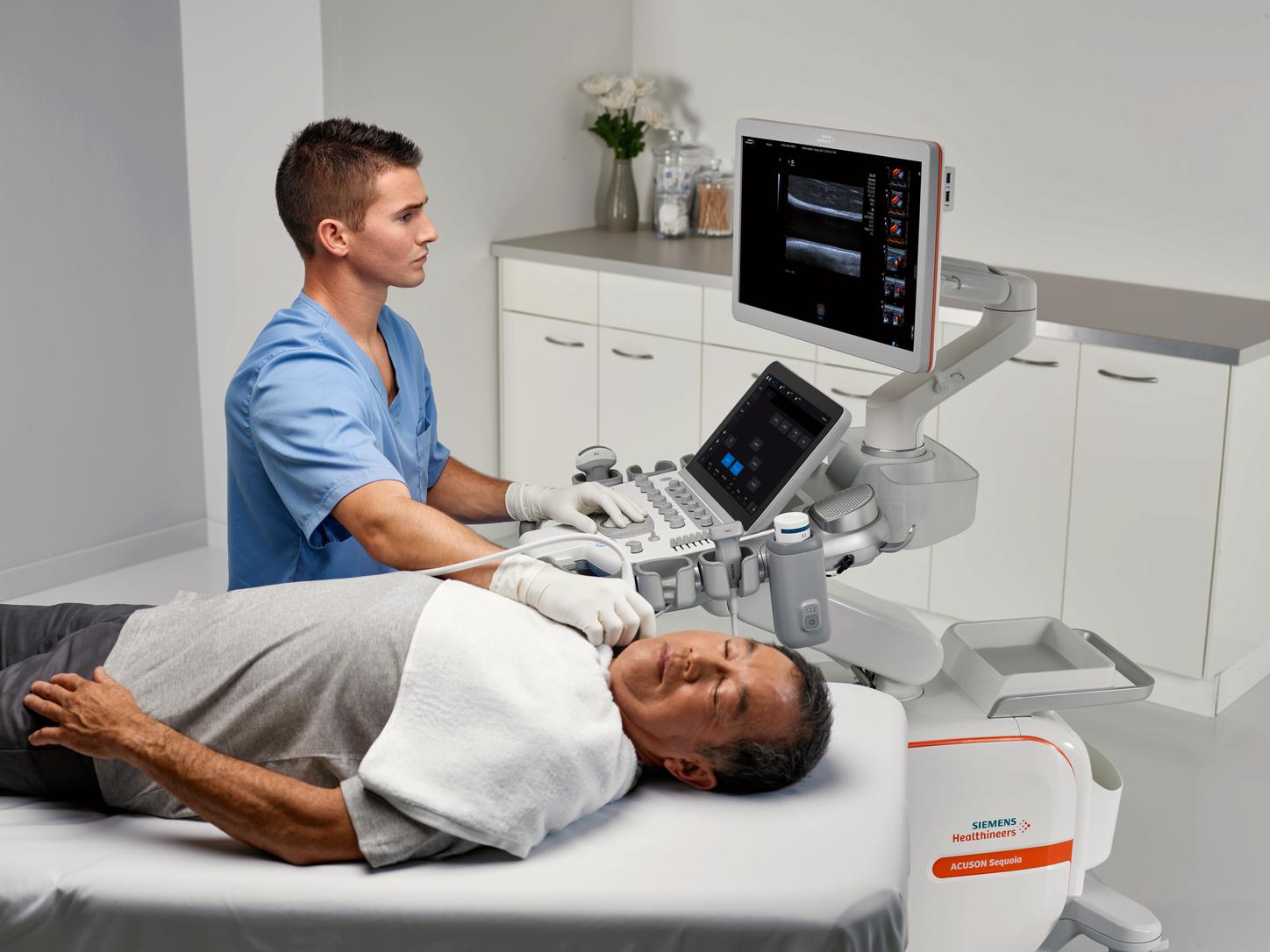
Non-invasive imaging for early detection and follow-up Ultrasound is a low-cost and non-invasive imaging exam that enables early detection and follow-up for stroke patients
Ultrasound Methods are useful in Stroke prevention in many ways, can also be used to assess plaque vulnerability, by detecting echolucency, ulceration and plaque heterogenicity on assessment of plaque texture.
- Point-of-Care Ultrasound. Many ultrasound systems can perform Transcranial Doppler (TCD) examination. TCD can be utilized in the field to diagnose many ischemic strokes. Traditional TCD exams are time intensive, performed by a specialist to look at the entire vasculature of the brain through multiple windows.
- The use of Carotid Ultrasound in the Coronary Artery Disease Screening results in a high prevalence of coronary artery disease and high probabilities of coronary angiography and revascularization, and thus it is a useful and feasible strategy for the screening of asymptomatic patients.
- Transcranial ultrasound may broaden the abilities of stroke neurologists to rapidly evaluate by assessing hemodynamic changes and reperfusion in stroke patients.
Our ACUSON Ultrasound offers the technology you need for confident stroke assessment.

Clear image quality for confident diagnosis and treatment
To quickly and confidently diagnose stroke, assess its impact, and perform mechanical thrombectomy, you need clear information. All our CT and MRI scanners as well as angiography systems let you see even small anatomical details in excellent quality. See for yourself!*

MAGNETOM Vida: Standard stroke protocol
example of hemorrhage visualization


Native syngo DynaCT Sine Spin
syngo DynaCT Sine Spin improves the image quality of cranial Flat-Detector CT (FDCT) scans, especially in the posterior fossa and the basal part of the skull. syngo DynaCT Sine Spin reduces artifacts caused by bony structures.
SPINNERS
Siemens Healthineers is the grant giver of the investigator-initiated SPINNERS study, a clinical trial planned and performed by Prof. Marios-Nikos Psychogios, University Hospital Basel, Switzerland and Dr. Adam S. Arthur, University of Tennessee Health Sciences Center and Semmes-Murphey Clinic, Memphis, US.
The study is designed to evaluate whether FDCT imaging with syngo DynaCT Sine Spin has likewise high diagnostic accuracy compared to Multi-Slice CT (MSCT) in detecting intracranial bleeding.
Find out more: Official Study Registry
Read more about the clinical investigators: One stop in stroke

syngo DynaCT Multiphase
 AP projection
AP projection Lateral projection
Lateral projectionFollow-up DSA to visualize treatment success

- Follow-up syngo DynaCT after clipping, with intravenous contrast media injection
- Axial maximum intensity projection of the clipped aneurysm

- Follow-up syngo DynaCT after clipping, with intravenous contrast media injection
- Dual-volume vessel presentation of the clipped aneurysm

Native head scan
Assist with or support differential diagnosis of acute stroke with excellent gray-white matter differentiation and contrast enhancement

Perfusion scan
Evaluation of infarct core and penumbra by automatically providing perfusion maps for further treatment decisions

Angiography
CT planning of the following treatment with definition of occlusion length and collateral status and automated bone removal

syngo.CT DE Brain Hemorrhage
Discriminate hemorrhage from iodine uptaking lesions

Cinematic VRT
Clearly visualize clots and get photorealistic and easy-to-understand material for education, publication, and communication

Bone removal solutions
Available for different acquisition techniques for automatic case preparation, image pre-processing, and prior study pre-fetching

GOBrain1) allows push-button brain exams in 5 minutes2)
1) Prakkamakul et al. “Ultrafast brain MRI: Clinical deployment and comparison to conventional brain MRI at 3T.” J of Neuroimaging 2016
2) MAGNETOM Skyra, Head 32 coil. Exam times will vary.

MAGNETOM Sola: T1 contrast sagittal MPRAGE

MAGNETOM Vida: Standard stroke protocol
example of hemorrhage visualization


Native syngo DynaCT Sine Spin
syngo DynaCT Sine Spin improves the image quality of cranial Flat-Detector CT (FDCT) scans, especially in the posterior fossa and the basal part of the skull. syngo DynaCT Sine Spin reduces artifacts caused by bony structures.
SPINNERS
Siemens Healthineers is the grant giver of the investigator-initiated SPINNERS study, a clinical trial planned and performed by Prof. Marios-Nikos Psychogios, University Hospital Basel, Switzerland and Dr. Adam S. Arthur, University of Tennessee Health Sciences Center and Semmes-Murphey Clinic, Memphis, US.
The study is designed to evaluate whether FDCT imaging with syngo DynaCT Sine Spin has likewise high diagnostic accuracy compared to Multi-Slice CT (MSCT) in detecting intracranial bleeding.
Find out more: Official Study Registry
Read more about the clinical investigators: One stop in stroke

syngo DynaCT Multiphase
 AP projection
AP projection Lateral projection
Lateral projectionFollow-up DSA to visualize treatment success

- Follow-up syngo DynaCT after clipping, with intravenous contrast media injection
- Axial maximum intensity projection of the clipped aneurysm

- Follow-up syngo DynaCT after clipping, with intravenous contrast media injection
- Dual-volume vessel presentation of the clipped aneurysm

Native head scan
Assist with or support differential diagnosis of acute stroke with excellent gray-white matter differentiation and contrast enhancement

Perfusion scan
Evaluation of infarct core and penumbra by automatically providing perfusion maps for further treatment decisions

Angiography
CT planning of the following treatment with definition of occlusion length and collateral status and automated bone removal

syngo.CT DE Brain Hemorrhage
Discriminate hemorrhage from iodine uptaking lesions

Cinematic VRT
Clearly visualize clots and get photorealistic and easy-to-understand material for education, publication, and communication

Bone removal solutions
Available for different acquisition techniques for automatic case preparation, image pre-processing, and prior study pre-fetching

GOBrain1) allows push-button brain exams in 5 minutes2)
1) Prakkamakul et al. “Ultrafast brain MRI: Clinical deployment and comparison to conventional brain MRI at 3T.” J of Neuroimaging 2016
2) MAGNETOM Skyra, Head 32 coil. Exam times will vary.

MAGNETOM Sola: T1 contrast sagittal MPRAGE

MAGNETOM Vida: Standard stroke protocol
example of hemorrhage visualization



 AP projection
AP projection Lateral projection
Lateral projection










Stroke partnerships around the world

Australia
Asia
Europe
North America

Vietnam
Transforming stroke care delivery
Stroke International Services (SIS)Stroke International Services (SIS) and Siemens Healthineers enter into a partnership to advance stroke management in Vietnam Stroke International Services (SIS) and Siemens Healthineers have entered into an 8-year Value Partnership to advance stroke management in Vietnam. As part of this long-term partnership, Siemens Healthineers will install innovative medical technology and robotic solutions, anchoring on various digitalization platforms, and will further develop its training centers to organize customized education programs on managing stroke, moving forward. This investment by SIS will focus on building a full stroke management network, with an extension to Ho Chi Minh city and Quang Nam province. For Siemens Healthineers, this will be the first Value Partnership focusing on stroke in Southeast Asia.
Customer case studies
7%1
Inpatient length of stay
- As part of our Value Partnership to reshape healthcare delivery, Medical University South Carolina (MUSC), USA and Siemens Healthineers aim to optimize stroke care within the community
- 7% reduction in inpatient length of stay for ischemic patients1
Optimized scheduling
- Optimize scheduling in new neuro-interventional area through digital twin-enhanced workflow simulation
Pioneer robotic capability3
Future value creation:
- Collaboration to pioneer neuro-interventional robotic capability
- Explore implementation of artificial intelligence to guide providers during thrombectomy
33%1
Improve outcome and quality of life for stroke patients
Consulting for optimization of clinical processes and workflows
- State-of-the-art imaging modalities to advance clinical capabilities and drive reputation
- 33% reduction in the degree of severity of symptoms at discharge1
27%1
Faster treatment
Optimize processes to shorten door-to-groin times
- Support during the planning and construction phase. Site planning taking into account process efficiency aspects and on-site coordination via dedicated project manager
- 27% reduction in door-to-groin time1
11%1
Reduction in cost per case
Increase overall profitability
- Asset and fleet optimization via IT analytics to standardize quality of care and ensure maximized returns
- 11.2% reduction in cost per case while number of cases increased by 15.1%1
Education

The role of imaging along the stroke pathway - clincal case studies
Explore how advanced imaging technologies, including MRI, CT, and angiography, are transforming stroke care across diverse clinical settings. From high-field to lower-field MRI systems these case studies highlight the pivotal role of imaging in identifying stroke type, location, and extent. Discover how these innovations are guiding treatment decisions and potentially reducing the risk of lasting damage.
Clinical trials on stroke
In recent years, various clinical trials have shown the advantages of performing endovascular thrombectomy in patients with a high stroke score as well as of one-stop stroke care.

The WAKE-UP trial shows favorable outcomes for acute ischemic stroke patients with an unknown stroke onset: Patients identified by DWI-FLAIR mismatch on MRI with subsequent thrombolysis had significantly better functional outcomes than the placebo group.7

The DAWN trial shows that time alone shouldn’t be a disqualifier for endovascular thrombectomy. For example: 48.6% of patients in the thrombectomy group experienced less disability, compared to 13% in the control group who received standard medical care.4

DEFUSE 3 shows favorable outcomes for late-window patients. For example: Mortality rate was 14% in the endovascular therapy group, compared to 26% in the medical therapy group. And there was no significant between-group difference in adverse events.4

ESCAPE trial “Among patients with acute ischemic stroke with a proximal vessel occlusion, a small infarct core, and moderate-to-good collateral circulation, rapid endovascular treatment improved functional outcomes and reduced mortality.” (from the publication)5

In their study, M. Psychogios et al. have shown that diagnosing and treating potential LVO patients on one system can save valuable time and significantly improve functional outcome.6

The WAKE-UP trial shows favorable outcomes for acute ischemic stroke patients with an unknown stroke onset: Patients identified by DWI-FLAIR mismatch on MRI with subsequent thrombolysis had significantly better functional outcomes than the placebo group.7

The DAWN trial shows that time alone shouldn’t be a disqualifier for endovascular thrombectomy. For example: 48.6% of patients in the thrombectomy group experienced less disability, compared to 13% in the control group who received standard medical care.4

DEFUSE 3 shows favorable outcomes for late-window patients. For example: Mortality rate was 14% in the endovascular therapy group, compared to 26% in the medical therapy group. And there was no significant between-group difference in adverse events.4

ESCAPE trial “Among patients with acute ischemic stroke with a proximal vessel occlusion, a small infarct core, and moderate-to-good collateral circulation, rapid endovascular treatment improved functional outcomes and reduced mortality.” (from the publication)5

In their study, M. Psychogios et al. have shown that diagnosing and treating potential LVO patients on one system can save valuable time and significantly improve functional outcome.6

The WAKE-UP trial shows favorable outcomes for acute ischemic stroke patients with an unknown stroke onset: Patients identified by DWI-FLAIR mismatch on MRI with subsequent thrombolysis had significantly better functional outcomes than the placebo group.7





Did this information help you?
Thank you.
The products/features mentioned herein are not commercially available in all countries. Their future availability cannot be guaranteed.
The statements by Siemens Healthineers’ customers described herein are based on results that were achieved in the customer's unique setting. Because there is no “typical” hospital or laboratory and many variables exist (e.g., hospital size, samples mix, case mix, level of IT and/or automation adoption) there can be no guarantee that other customers will achieve the same results.
https://www.strokeforum.com/overview/epidemiology
Planned future value creation
G. Thomalla et al., "MRI-Guided Thrombolysis for Stroke with Unknown Time of Onset"; N Engl J Med 2018; 379:611-622

