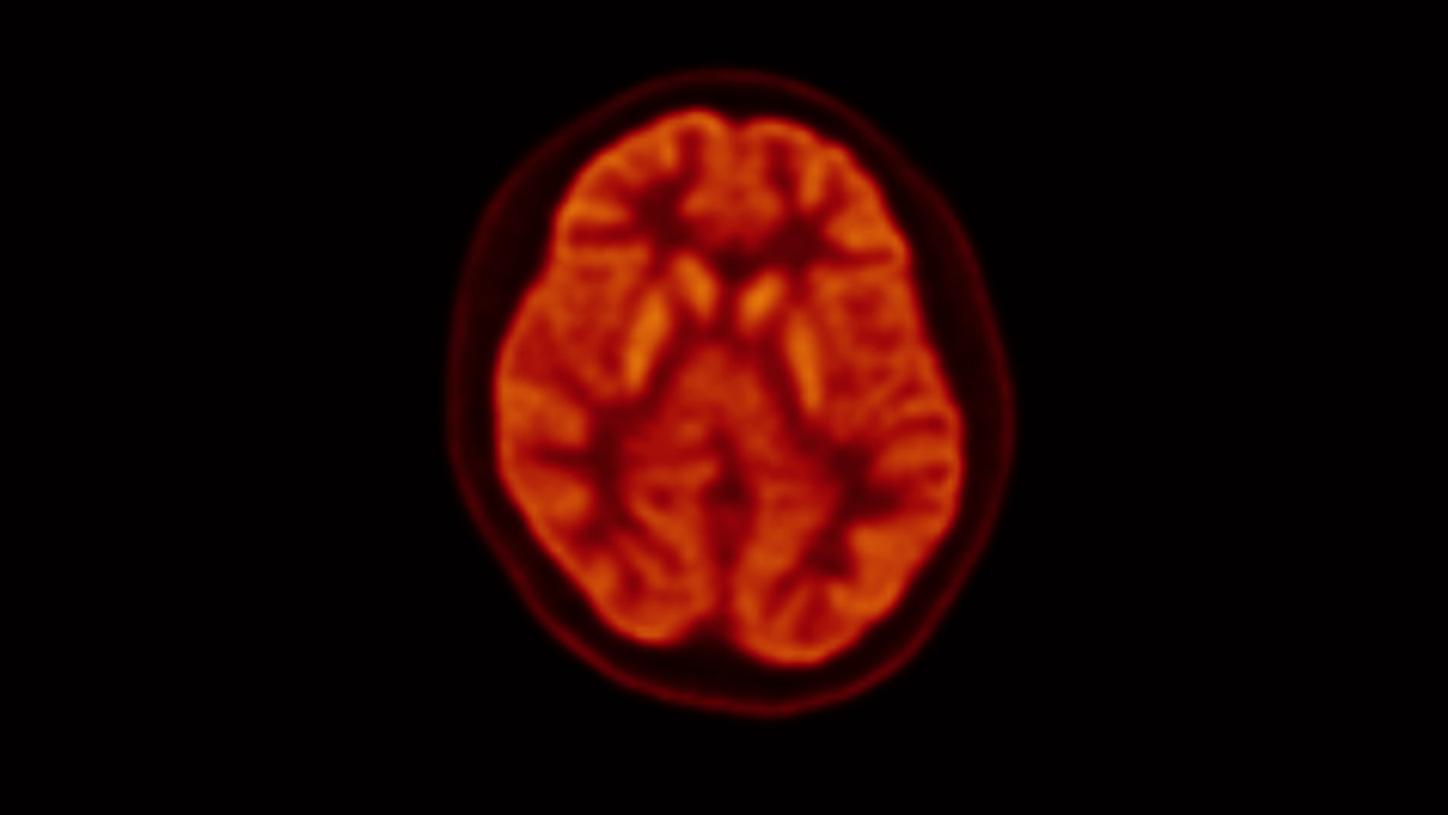
Neurologic PET
Exploring neurological indications in PET and PET/CT
PET brain imaging provides a functional assessment and observes brain activity and metabolic processes. PET effectively detects beta-amyloid plaque, tau deposits, glucose or amino acid metabolism, and dopamine receptors in the brain.1 PET brain imaging can often detect changes in brain function and metabolism before other conventional imaging modalities like MRI or CT scans. Early detection can be vital for diagnosing neurological conditions sooner when interventions may be more effective. Alzheimer's Disease, Parkinson's Disease, and Epilepsy are common indications for PET neuroimaging.
Did this information help you?
All rights reserved. All product/company names mentioned herein are the trademarks of their respective owners
Lattanzi S, Brigo F, Vernieri F, Silvestrini M. Visit-to-visit variability in blood pressure and Alzheimer's disease. J Clin Hypertens (Greenwich). 2018 May;20(5):918-924. doi: 10.1111/jch.13290. Epub 2018 Apr 25. PMID: 29693801; PMCID: PMC8031352.
Alzheimer’s Association, 2021 Alzheimer’s Disease Facts and Figures, Alzheimer’s Dement 2021; 17(3)
Mayo Clinic Staff. “Alzheimer's Stages: How the Disease Progresses.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 29 Apr. 2021, https://www.mayoclinic.org/diseases-conditions/alzheimers-disease/in-depth/alzheimers-stages/art-20048448.
Mayo Clinic Staff. “Learn How Alzheimer's Is Diagnosed.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 7 May 2022, https://www.mayoclinic.org/diseases-conditions/alzheimers-disease/in-depth/alzheimers/art-20048075.
Bateman, Randall J., et al. "Clinical and biomarker changes in dominantly inherited Alzheimer's disease." N Engl J Med 367 (2012): 795-804.
Alzheimer’s Association. (2021). Alzheimer’s disease facts and figures. [Ebook]. Chicago. Retrieved from https://alz.org/media/Documents/alzheimers-facts-and-figures-2021.pdf
“Alzheimer's Disease Fact Sheet.” National Institute on Aging, U.S. Department of Health and Human Services, https://www.nia.nih.gov/health/alzheimers-disease-fact-sheet.
Lattanzi S, Brigo F, Vernieri F, Silvestrini M. Visit-to-visit variability in blood pressure and Alzheimer's disease. J Clin Hypertens (Greenwich). 2018 May;20(5):918-924. doi: 10.1111/jch.13290. Epub 2018 Apr 25. PMID: 29693801; PMCID: PMC8031352.
Chen B, Marquez-Nostra B, Belitzky E, et al. PET Imaging in Animal Models of Alzheimer's Disease. Front Neurosci. 2022;16:872509. Published 2022 May 24. doi:10.3389/fnins.2022.872509
FOR HEALTHCARE PROFESSIONALS Frequently asked questions about beta-amyloid imaging. (2021) https://www.alz.org/media/documents/health-care-pros-faqs-beta-amyloid-imaging.pdf
“About Us New IDEAS Study.” About Us, https://www.ideas-study.org/About-Us#:~:text=The%20New%20IDEAS%20study%20will%20also%20have%20two%20additional%20objectives,have%20consented%20to%20blood%20collection.
“Monoclonal Antibodies Directed against Amyloid for the Treatment of Alzheimer's Disease.” CMS.gov Centers for Medicare & Medicaid Services, https://www.cms.gov/medicare-coverage-database/view/ncacal-decision-memo.aspx?proposed=Y&NCAId=305.
Kumar A, Chugani HT. The role of radionuclide imaging in epilepsy, Part 1: Sporadic temporal and extratemporal lobe epilepsy. J Nucl Med. 2013;54(10):1775-1781. doi:10.2967/jnumed.112.114397
Hodolic M, Topakian R, Pichler R. (18)F-fluorodeoxyglucose and (18)F-flumazenil positron emission tomography in patients with refractory epilepsy. Radiol Oncol. 2016;50(3):247-253. Published 2016 Jul 19. doi:10.1515/raon-2016-0032
“4 Types of Epilepsy, Their Symptoms, and Treatments.” Medical News Today, MediLexicon International, https://www.medicalnewstoday.com/articles/types-of-epilepsy#contacting-a-doctor.
Sarikaya I. PET studies in epilepsy. Am J Nucl Med Mol Imaging. 2015;5(5):416-430. Published 2015 Oct 12
Fisher, Dr. Robert S, et al. “Operational Claissification of Seizure Types by the International League Against Epilepsy’ Position Paper of the ILAE Commission for Classification and Terminology.” Https://Onlinelibrary.wiley.com/Doi/Epdf/10.1111/Epi.13670, Wiley Online Library, 8 Mar. 2017, https://onlinelibrary.wiley.com/doi/epdf/10.1111/epi.13670.
Stanescu, Luana, et al. “FDG Pet of the Brain in Pediatric Patients: Imaging Spectrum with MR Imaging Correlation.” RadioGraphics, 30 Aug. 2013, https://pubs.rsna.org/doi/10.1148/rg.335125152.
CMS.GOV. “FDG Pet for Refractory Seizures.” CMS.gov Centers for Medicare & Medicaid Services, https://www.cms.gov/medicare-coverage-database/view/ncd.aspx?NCDId=294&NCDver=1.