Lung Cancer is the cancer with a very high mortality rate. Sebastian Schmidt, Head of Strategy and Medical Affairs CT at Siemens Healthineers, talks about early diagnosis and screening programs.
Watch the full video here.
Lung cancer is the #1 in cancer mortality, with 80%1 5-year-mortality. As the early stages of the disease are painless, the majority of diagnoses happen in late stages. Today, around 80% of the patients are diagnosed in stage 3/4, where only palliative treatment is possible.
Personalized screening of high risk groups with low-dose-CT is a way to significantly decrease lung cancer mortality. In current lung screening programs, around 80%2 of the patients are diagnosed in stage I or II, which allows treating them with curative intent.
There are, however, some concerns which hinder the implementation of screening programs: (1) Radiation Dose, (2) accuracy (false positives and negatives) and (3) costs and workload for medical personnel.
Our contribution
We as Siemens Healthineers actively address these three challenges and contribute to successfully implementing screening programs:
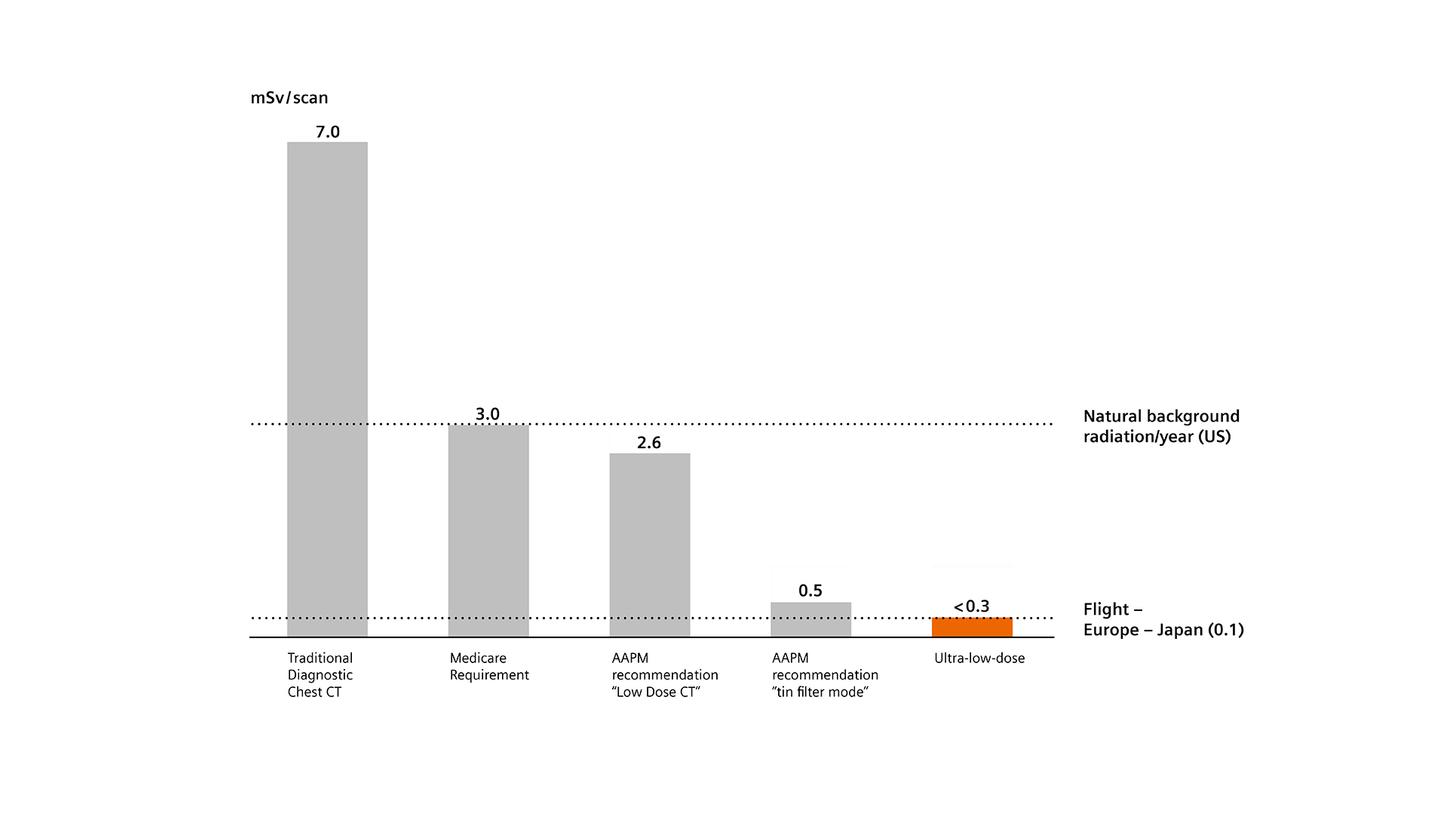
Radiation Dose
We provide ultra-low-dose CT technology that allows a screening examination much below the natural background radiation.
Accuracy
We provide AI tools that improve accuracy and at the same time reduce radiology workload (costs).
Costs and workload
We offer the ultra-low-dose technology even in the most cost-efficient CT scanners, making screening cost-effective, affordable and available to large patient populations, without compromising quality.