August 26, 2015 | The success of device therapies in cardiology depends on the correct placement of cardiac electrodes. At Hospital Wels-Grieskirchen in Austria, cardiac resynchronization therapy devices for heart failure patients are implanted based on 3D visualization of the coronary sinus. This decreases the risk of therapy failure.
Text: Philipp Grätzel von Grätz
Photos: Detlef Schneider

Cardiac resynchronization therapy (CRT) is a highly effective treatment to improve both the symptoms and prognosis of patients with chronic heart failure. Established in the early 2000’s1, nowadays it is an indispensable treatment option for heart failure patients, says Marcus Ammer, MD, Head of Electrophysiology at Hospital Wels-Grieskirchen in Austria: “CRT improves breathlessness and exercise capacity, but it also reduces hospitalizations and mortality.”
Increasing Efficiency of the Pumping Heart
What CRT devices do is to increase the efficiency of the pumping heart: They re-coordinate or “resynchronize” the beating of the two cardiac ventricles. To this end, a pacemaker-like device is placed below the skin, and three electrodes are implanted. Two of them are inserted via the subclavian vein into the right atrium and the right ventricle, very similar to a conventional pacemaker implantation.

The Clinical Challenge
The third electrode or “left-ventricular lead” is more complex to put in place. It needs to rest in one of the coronary veins directly adjacent to the wall of the left ventricle.To get there, cardiologists have to locate the coronary sinus in the right atrium, the region where all coronary veins end, and identify the vein that best meets their needs. If the CRT implantation is successful, the two ventricles contract in a more coordinated fashion afterwards. Cardiac function improves, and heart failure symptoms are alleviated.
Widespread Use of CRT
“When we implant a CRT device, we strictly follow European guidelines,” says Michael Porodko, MD, who is responsible for CRT implantations. “We strongly believe that patients benefit most from cardiac resynchronization therapy when they are in chronic heart failure NYHA II – III and present with left bundle-branch block with a QRS-complex width of more than 150 msec.” According to international data, these criteria are met in around 1 in 5 to 1 in 10 patients with chronic heart failure. These are significant numbers. Taken together, in Europe and the U.S., more than 150,000 CRT devices are implanted every year.
Benefits for Patients are Different
Not every patient benefits, however. Studies have shown that for 3 out of 10 patients cardiac function does not improve after CRT implantation. “A correct placement of the left-ventricular lead is a major factor for a good treatment response,” says Porodko. “We know that success rates are highest if the LV lead is placed in the posterolateral part of the left ventricle. And we also know that patients with ischemic heart disease have lower response rates than patients with dilative cardiomyopathy.”
Reducing the Risk of Non-Response
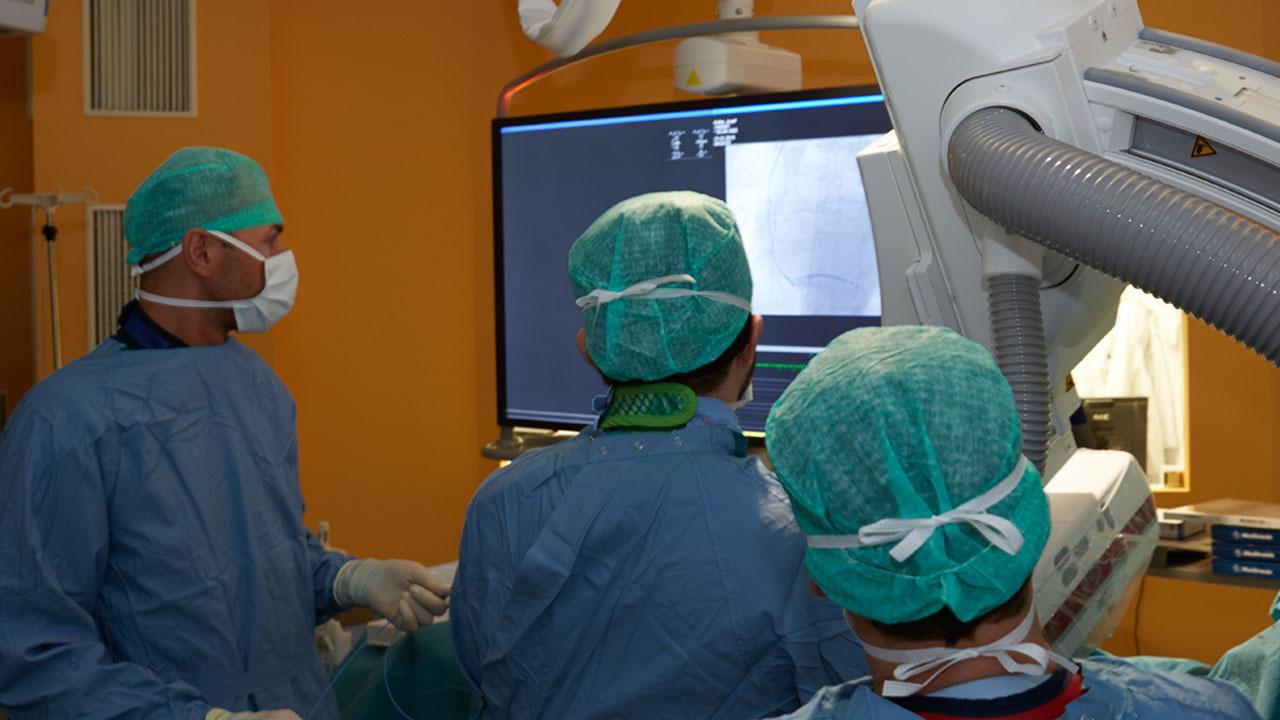
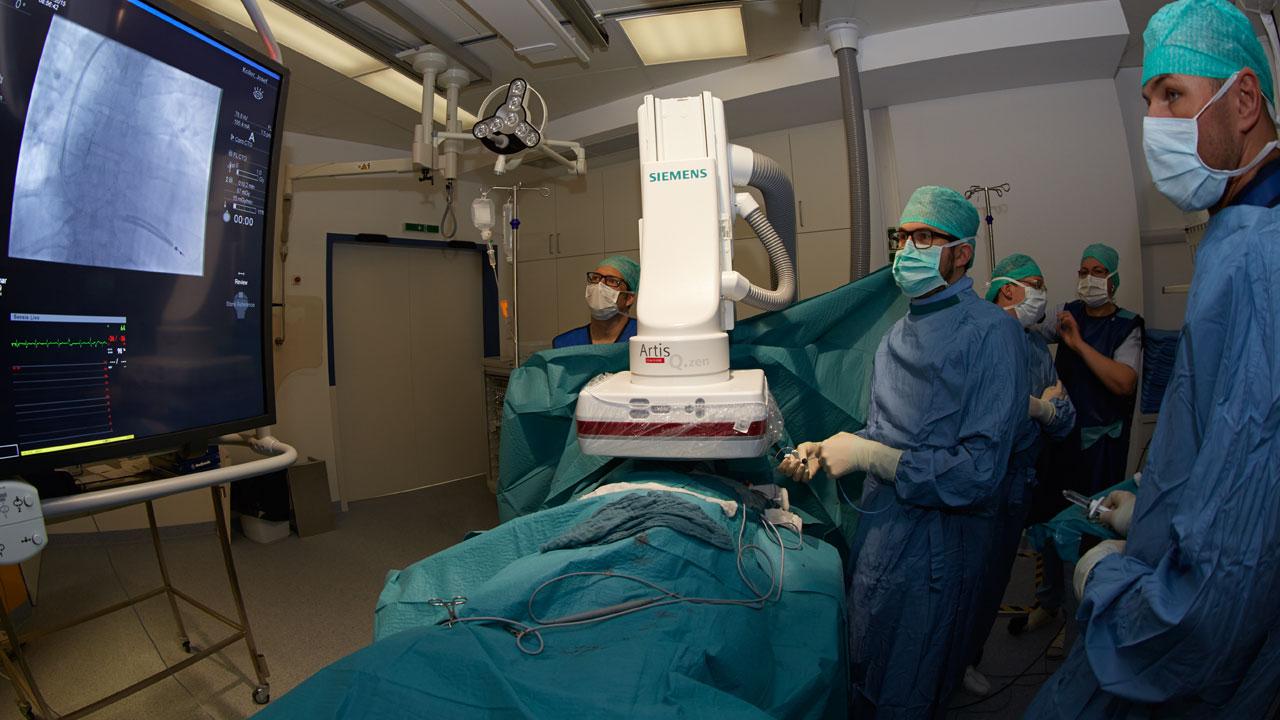
At Hospital Wels-Grieskirchen, the electrophysiological department has recently acquired a Siemens Artis Q.zen angiography system with the syngo DynaCT Cardiac application for rotational angiography. The system enables patients and operators to benefit from peri-operative 3D visualization of the cardiac anatomy in the angio suite. Porodko relies on it to optimize LV lead placement in CRT implantations. “What we do is to acquire a DynaCT run during CRT implantation in order to obtain a 3D reconstruction of the coronary sinus and its side branches,” explains Porodko. The 3D reconstruction of the coronary sinus is superimposed on the live fluoroscopy images. “This allows us to identify the most suitable cardiac vein quickly and to place the lead more accurately. Ultimately, this should reduce the risk of non-response.”
Shorter Intervention Time
Another benefit is the decreased implantation time: “We are actually faster than with the conventional implantation technique,” says Porodko. The main reason for this is a new syngo DynaCT protocol that was introduced in the summer of 2014. Hospital Wels-Grieskirchen was in fact the first hospital worldwide to work with this new protocol. It allows 3D visualization of the coronary sinus morphology derived from just one run of the rotational angiography system. This takes no more than five seconds.
The Process of Data Acquisition
Such quick data acquisition is possible because of rapid electrical pacing of the right ventricle, explains Ammer: “The rapid pacing prevents the ventricle from beating for exactly the five seconds that are needed for the DynaCT run. We don’t need any adenosine and we don’t need an ECG trigger.” During the rapid pacing, patients don’t need to lift their arms above their head anymore and they tolerate the procedure very well. There is a brief decrease in blood pressure, but right after the rapid pacing ends, circulation parameters return to normal.
Minimizing the Number of Non-Responders
“This works even in patients with severe heart failure,” says Ammer. “It is easy to do, since we don’t need an additional lead. For the rapid pacing, we use the right-ventricular lead of the CRT system.” Cardiologists all over the world have in fact gained substantial experience with this temporary electrical silencing of the heart in recent years. Rapid ventricular pacing is well established in transcatheter aortic valve implantations (TAVI), so more and more cardiologists are familiar with it. Ultimately, Ammer and Porodko hope that 3D visualization of the coronary sinus will help them to keep the rate of non-responders as low as possible.
Patient Selection is Key
In addition to advanced imaging for increased accuracy in lead placement, patient selection is key to the success of CRT treatment. In recent revisions, guidelines have become increasingly precise about which patients are suitable for CRT treatment. Quadripolar LV leads are another way to increase success rates. They are used routinely at Hospital Wels-Grieskirchen. If electric stimulation can be applied in different sections of the left-ventricular myocardium, the likelihood of a successful resynchronization increases. According to Porodko: “Achieving high response rates in CRT treatment requires a combination of measures, but imaging is at the core. It allows us to work as precisely, as quickly, and as patient-friendly as possible.”
About the Author
Philipp Grätzel von Grätz is a medical doctor turned freelance writer and book author based in Berlin, Germany. His focus is on biomedicine, medical technology, health IT, and health policy.