History
A 3-year-old male patient, with a known double aortic arch (DAA), was presented to the hospital due to progressive dysphagia over the past 6 months. An esophageal compression was suspected and a chest CT angiography (CTA) was requested for further assessment.
Diagnosis
CTA images showed a DAA splitting off from the ascending aorta, forming a complete vascular ring, uniting posteriorly and then reforming the descending aorta. Both arches were patent, with no evidence of an atretic segment. The right arch was dominant. Each arch gave rise to ipsilateral separate carotid and subclavian arteries, according to the four-artery sign. The trachea and the esophagus were encircled in the vascular ring. The proximal esophagus was compressed by the left arch, the trachea was intact. There were no signs of a patent ductus arteriosus or any other cardiac anomaly. The patient underwent surgical ligation of the left arch as well as of the ligamentum arteriosum. His dysphagia significantly improved immediately after surgery. At a follow up four months later, he continued to do well with only minor complaints.

Courtesy of Radiology Department, Sírio Libanês Hospital, Sao Paulo, Brazil
Fig. 1: Axial images (Fig. 1a–1f, cranio-caudal) and a cVRT image (Fig. 1g) show a compressed and discontinued proximal esophagus at the level of the left aortic arch (orange arrows). It shifts from the left-posterior to the right-posterior to the trachea and reappears below the vascular ring (white arrows).

Courtesy of Radiology Department, Sírio Libanês Hospital, Sao Paulo, Brazil
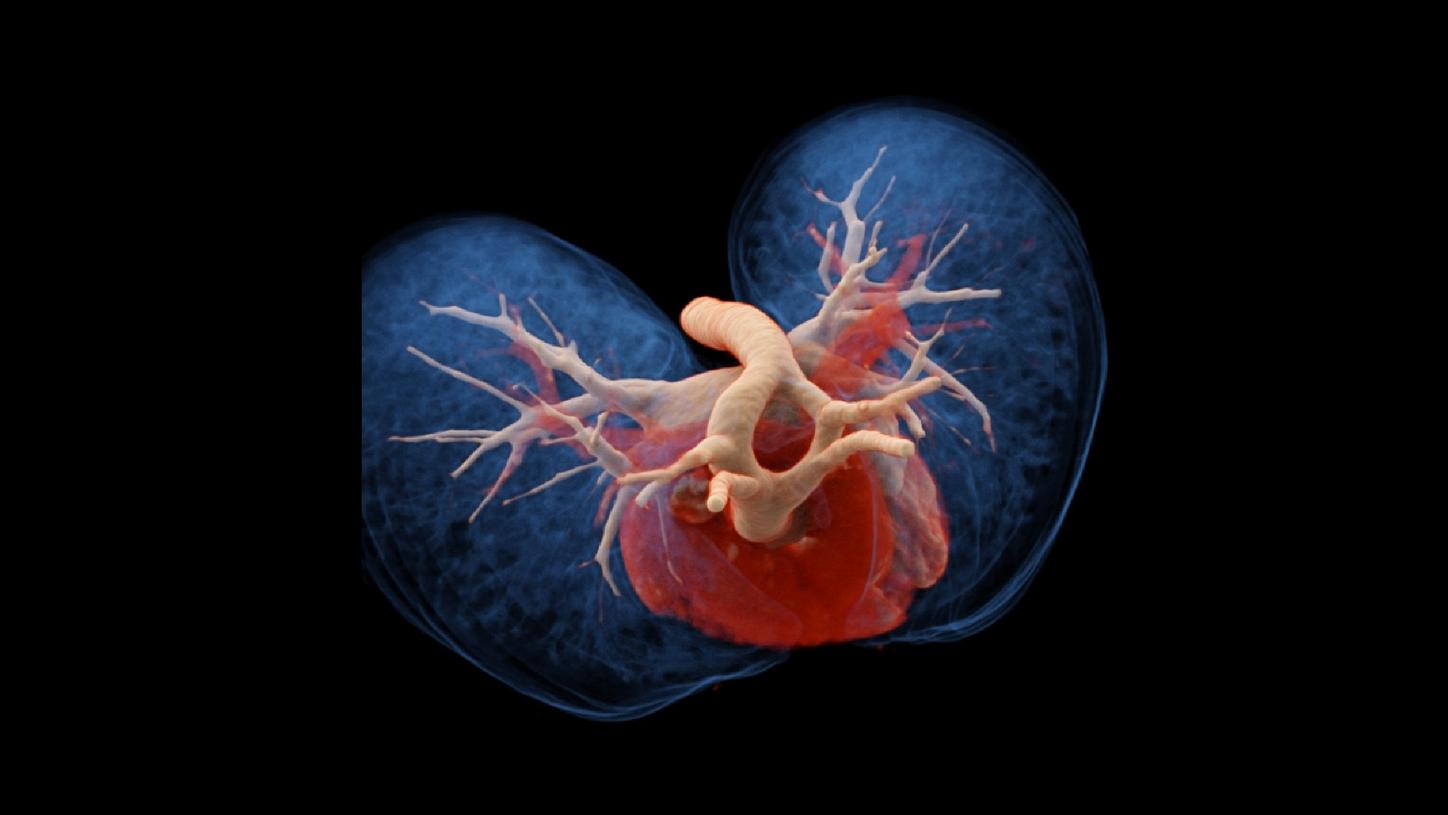
Fig. 2: cVRT images show a patent DAA, with the right dominant arch. Each arch gives rise to ipsilateral separate carotid and subclavian arteries, according to the four-artery sign.
Comments
DAA is a congenital vascular ring anomaly resulting from the lack of regression of the hypothetical embryologic double arch system. The two arches, encircling the trachea and the esophagus, may cause extrinsic compression, resulting in respiratory distress and/or feeding problems. Surgical correction is indicated in all symptomatic patients. CTA plays an imperative role in pre-operative assessment, defining the vascular anatomy in detail. However, obtaining cardiovascular images, without motion artifacts, is a challenge in pediatric cases. Motion artifacts are usually caused by the higher heart rate (125 bpm in this case) and the child’s inability of complying with the breathing instructions. To overcome these challenges, Turbo Flash, an innovative ultra-fast scanning technique, was designed for dual source scanner, SOMATOM Force, allowing for an acquisition speed of 737 mm/s. In this case, a total scan range of 13.4 cm is completed in just 0.25 s. Although the patient was sedated due to his extreme anxiety to the contrast injection, the scan was performed at free breathing. The optimal image quality achieved facilitates a confident diagnosis. The scanner also provides a high temporal resolution of 66 ms, which helps to freeze the heart motion. For a lifelike, three-dimensional demonstration of the complex anatomic details, cinematic volume rendering technique (cVRT) is applied, allowing for an intuitive understanding of spatial anatomical structures and easier communication on all sides.
Examination Protocol