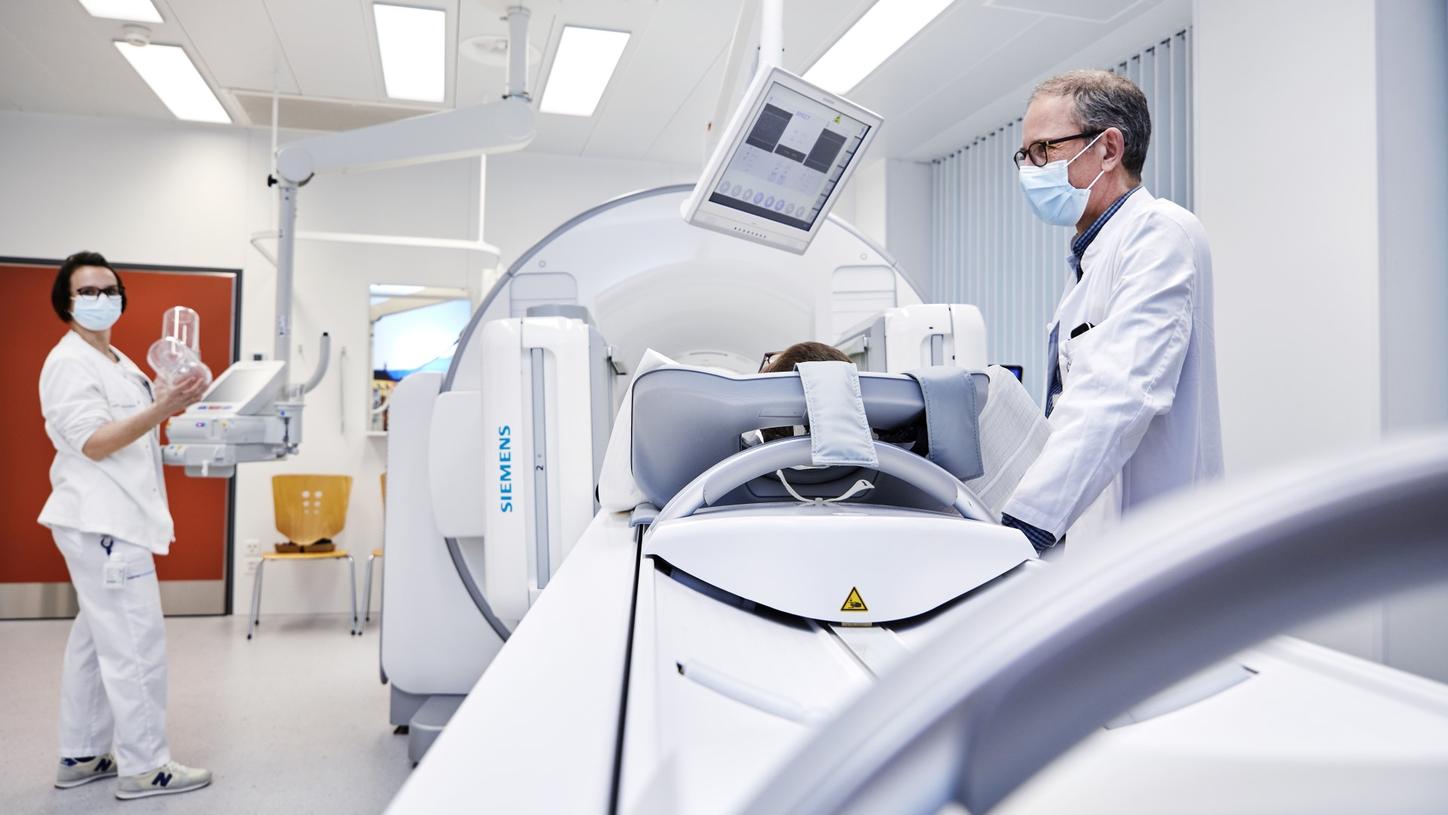
Since its introduction more than two decades ago, SPECT/CT imaging has seen significant technological advances that are expanding the modality’s power and accuracy. SPECT/CT expert Klaus Strobel from Lucerne Cantonal Hospital in Switzerland reveals how the method improves individual patient care and where he sees future clinical applications.
Photography by Raphael Zubler
Across the diagnostic imaging spectrum, SPECT and SPECT/CT have developed into staples that are depended upon to drive improved patient outcomes. With SPECT originating more than 50 years ago and evolving into SPECT/CT over two decades ago, these modalities continue to meet the challenges of today through the implementation of new features and methods of use, assisting physicians in the diagnosis and targeted care of each individual patient.
As a hybrid method, SPECT/CT combines single-photon emission computed tomography (SPECT), which provides metabolic information from injected radionuclides, with anatomical information of bones and organs obtained from computed tomography (CT). This unites the high sensitivity of SPECT with the specific physiological localization provided by CT. “This improves diagnostic accuracy for a wide range of clinical conditions compared to SPECT or CT imaging alone,” confirms Prof. Dr. Klaus Strobel, head of the nuclear medicine department at the Lucerne Cantonal Hospital, Switzerland.
Broad range of clinical applications
Located in a large center for nuclear medicine in central Switzerland, Strobel’s department is responsible for serving a population of around one million people. To enhance its diagnostic imaging capabilities, the department acquired two Symbia Intevo Bold™ SPECT/CT imaging scanners, one in 2019 and another in 2020, to replace its aging SPECT/CT scanners.
Strobel and his team—which includes three other physicians who are double board certified in radiology and nuclear medicine and 15 technologists who are also trained in both specialties—most frequently use SPECT/CT to investigate skeletal conditions like lesions of bone and joints. These experts also employ SPECT/CT for a broad range of other investigations, such as examinations of the thyroid and parathyroid glands, cardiac analysis to investigate perfusion and possible ischemia, and applications in the brain, for instance, on patients with suspected Parkinson’s disease. The team also explores the modality’s use for further clinical applications.
In fact, SPECT/CT has seen significant technological advances that have expanded the modality’s scope. First, the quality of scans has increased due to better CT hardware, which is, according to Strobel, probably the most significant advancement in recent years. Modern machines feature more rapidly rotating radiation sources and detectors with a greater number of slices resulting in the ability to provide clear and high-resolution images while simultaneously reducing imaging time.
"When investigating possible metastatic growth in prostate or breast cancer patients, a SPECT/CT measurement can reveal information about metastases in bones, while a back-to-back contrast CT provides information on possible tumors in the lung or liver."
One-stop imaging
To harness the SPECT/CT to its full capabilities, Strobel and his team are using Symbia Intevo Bold to provide what he refers to as “one-stop imaging.” His team routinely utilizes a contrast injector in conjunction with the CT. “When investigating possible metastatic growth in prostate or breast cancer patients, a SPECT/CT measurement can reveal information about metastases in bones, while a back-to-back contrast CT provides information on possible tumors in the lung or liver,” Strobel explains. He goes on to emphasize the importance of providing fused 3D images to the referring physicians and to patients, as it promotes the power of the imaging modalities.
In addition, the CT capabilities combined with image processing software allow Strobel and his co-workers to perform measurements they were unable to provide before. The experts can now add calcium scoring to cardiac perfusion SPECT/CT as an additional prognostic data point to assess the risk for relevant coronary artery disease and myocardial infarction.
Strobel’s team also applies unique Siemens Healthineers CT technologies like iMAR, the iterative algorithm for metal artifact reduction along with their SPECT/CT imaging techniques.
This helps the team apply diagnostic SPECT/CT for patients who underwent a knee or a hip replacement and therefore carry metal prostheses.
“Such metal components normally create hindering artifacts in CT images,” explains Strobel. A tailored image processing algorithm like iMAR reduces such artifacts and provides high-quality images of the tissue around metal protheses without any information being obscured. The iMAR images can be applied for attenuation correction to the SPECT images providing a dual benefit by enhancing the reconstructed image quality for both modalities.
Additionally, along with iMAR, Strobel and his co-workers regularly use dual-energy CT in patients with knee prothesis to increase visibility of subtle osteolysis at the metal-bone interface as a sign for early loosening.
Expanding the scope of SPECT/CT imaging
“Thanks to these technical advancements, we have certainly been able to improve diagnosis and patient care,” Strobel concludes. It’s no surprise that the use of SPECT/CT is steadily moving towards new clinical indications. Recently, Strobel’s team has begun working together with lymphatic surgeons to explore imaging of the lymphatic nodes and vessels. These experts are also investigating specialized applications with available tracers, such as imaging cardiac amyloidosis (a severe disease of the heart) using a tracer currently used for bone imaging. “I can imagine that more diagnosable indications will come up when researchers further investigate the scope of bone and joint SPECT/CT scans,” says Strobel. “We are still limited in imaging of soft tissues, and I see potential to improve in this area.” The Lucerne team invented “SPECT/CT arthrography,” a combination of CT arthrography with intraarticular contrast and SPECT as a new technique allowing the assessment of metabolic bone changes and cartilage or ligament lesions in one investigation in knee, ankle, or wrist disorders.
According to Strobel, a promising new perspective is the quantification of tracer uptake in the images, providing standard uptake values (SUV)—already being done in PET/CT measurements. Strobel appreciates the solution for quantification referred to as xSPECT Quant™. “I think it is important that tracer quantification can be done in SPECT/CT as easily as in PET/CT; that one can place a volume of interest (VOI) in the lesion and immediately obtain the SUV to compare with older images, such as for therapy response assessment.” Strobel also states, “This easy-to-use and precise tracer quantification tool was actually one of the main reasons for us to choose Symbia Intevo Bold, since it’s unique on the market.”
In fact, initial research results in the field indicate that tracer quantification may be used to guide treatment decisions or response to a given therapy.1,2 There is still much research to be done,” says Strobel, “but I think quantification in SPECT/CT will be an especially interesting application to explore in the future.”
Broader applications for the original features of SPECT/CT have continuously been revealed throughout the life cycle. With the addition of new imaging tools, medical professionals are discovering innovative ways to utilize SPECT/CT to deliver cutting-edge service for patients. The modality continues to advance, and the coming years promise to reveal new uses that will keep it at the forefront of nuclear medicine for decades to come.
About the author
Santina Russo is a freelance science journalist in Zurich, Switzerland.